Stent: What is a Stent?
Cardiovascular diseases are a major cause of illness and death globally. The use of Cardiovascular Support Devices is critical in managing these conditions. A Stent is a small, mesh-like tube used to keep arteries open. This improves blood flow and reduces the risk of heart attacks. Stents play a vital role in cardiovascular health, restoring blood flow and preventing future cardiac events.
This guide will offer a detailed look at stents. We will cover their types, benefits, and the latest advancements in cardiovascular support technology. Stents are vital medical devices for maintaining heart health. They support narrowed or weakened arteries, ensuring blood reaches the heart and vital organs without obstruction.
Definition and Basic Function
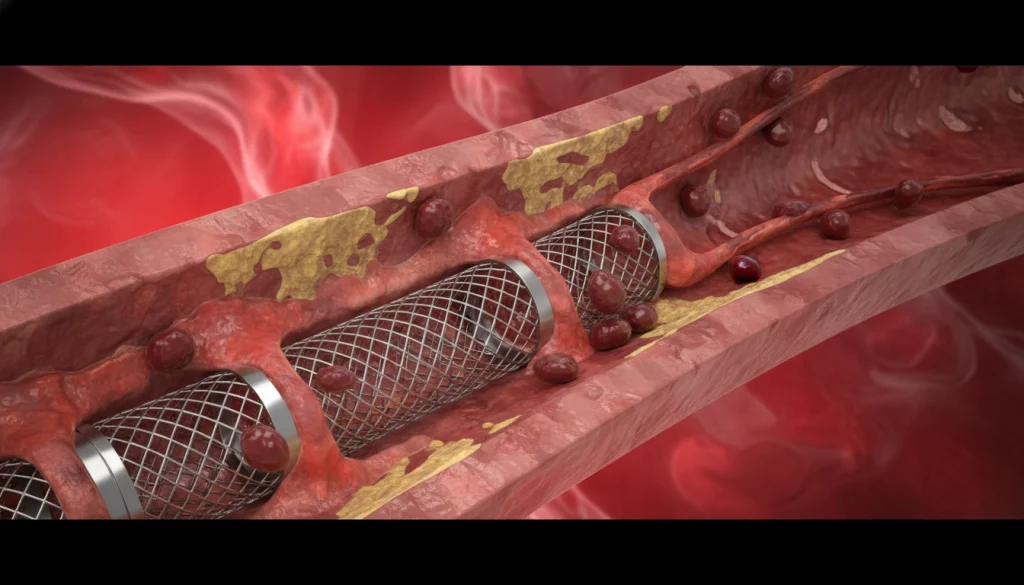
A stent is a small, mesh-like tube, often made of metal or other materials. Its main role is to keep arteries open, improving blood flow and lowering heart attack risks. During angioplasty, a minimally invasive procedure, the stent is placed in the affected area and expanded to support the artery walls.
Historical Development of Stents
The idea of stenting emerged in the 1960s, but the first stents were developed in the late 1980s. Initially, these stents were made of bare metal and prone to clotting. Advances in technology have led to drug-eluting stents, which significantly reduce clot formation and enhance long-term results. Today, stents are a key treatment for artery disease, providing a safe and effective solution.
The Evolution of Stent Technology
The journey of stent technology has been filled with milestones and breakthroughs. From simple beginnings to advanced devices, stents have become essential in treating heart conditions. Their evolution showcases the relentless pursuit of innovation in medical engineering.
Early Stent Designs
The initial stents were basic, often leading to complications like thrombosis and restenosis. These early models were crafted from materials not suited for long-term use. This led to numerous clinical hurdles.
Breakthrough Innovations
The advent of drug-eluting stents (DES) was a game-changer. They significantly cut down on in-stent restenosis rates. This innovation made stenting safer and more effective, marking a significant shift in stent technology’s history.
Modern Stent Engineering
Now, stent technology is advancing with the introduction of bioresorbable vascular scaffolds (BVS) and other cutting-edge materials. Modern engineering aims to enhance deliverability, safety, and effectiveness. This ensures stents remain a cornerstone in cardiovascular disease treatment.
The continuous evolution of stent technology promises to improve patient outcomes. It also broadens the scope of stenting in treating various medical conditions.
Types of Stents
The evolution of stent technology has given rise to a wide array of stent types. Each is crafted to meet specific vascular needs. This variety is essential for effectively treating various cardiovascular conditions.
Bare Metal Stents (BMS)
Bare Metal Stents, the first stent design, are constructed from stainless steel or other metals. They offer mechanical support to keep arteries open. Yet, they lack coatings or medications that newer stents have.
Compared to newer stent designs, BMS carry a higher risk of in-stent restenosis. Despite this, they remain applicable in certain clinical scenarios.
Drug-Eluting Stents (DES)
Drug-Eluting Stents mark a significant leap forward in stent technology. They are coated with medications that release slowly. This prevents cell proliferation and significantly reduces the risk of restenosis.
First-Generation DES
The advent of the first-generation DES ushered in a new era for coronary stenting. These stents saw a notable decrease in restenosis rates compared to BMS.
Second-Generation DES
Second-generation DES have built upon the first with newer drugs, more biocompatible polymers, and advanced delivery systems. These enhancements have further minimized complications.
Bioresorbable Vascular Scaffolds (BVS)
Bioresorbable Vascular Scaffolds represent a newer stent category. They gradually dissolve after fulfilling their purpose. Made from materials the body can absorb, they aim to reduce long-term complications.
The goal of BVS is to restore normal vessel function and diminish the need for future interventions.
Specialized Stent Varieties
Aside from the main categories, there are specialized stents for specific conditions or anatomical locations. These include stents for peripheral artery disease and carotid artery stenosis.
These specialized stents underscore the continuous innovation in stent technology. They are designed to address a wide range of medical needs.
Medical Conditions Requiring Stent Placement
Several cardiovascular conditions necessitate stent placement to restore normal blood flow. Stents, small, mesh-like tubes, keep arteries open. This improves blood circulation to vital organs and tissues. The use of stents is a critical treatment for various vascular diseases.

Coronary Artery Disease
Coronary artery disease (CAD) is a common condition treated with stents. CAD occurs when coronary arteries, which supply blood to the heart muscle, become narrowed or blocked. This can lead to reduced blood flow to the heart, causing chest pain or other symptoms.
Acute Coronary Syndrome
Acute coronary syndrome (ACS) is a serious condition that includes heart attack and unstable angina. Stent placement is often used in emergency situations. It quickly restores blood flow to the heart, minimizing damage to the heart muscle.
Stable Angina
Stable angina is characterized by chest pain or discomfort when the heart muscle does not receive enough oxygen-rich blood. Stents can alleviate symptoms by improving blood flow through the coronary arteries. This reduces the frequency and severity of angina episodes.
Peripheral Artery Disease
Peripheral artery disease (PAD) involves the narrowing or blockage of peripheral arteries, often in the legs. Stent placement can restore blood flow, reducing symptoms such as leg pain during walking. Improved circulation promotes wound healing and reduces infection risk.
Carotid Artery Stenosis
Carotid artery stenosis refers to the narrowing of the carotid arteries in the neck, which supply blood to the brain. Stenting can prevent stroke by keeping these arteries open. This reduces the risk of brain damage due to lack of blood flow.
Non-Vascular Applications
While stents are commonly associated with vascular conditions, they are also used in non-vascular applications to treat various other medical conditions.
Biliary Stents
Biliary stents are used to keep the bile ducts open, allowing bile to flow from the liver to the intestine. This is often necessary in cases of bile duct obstruction due to cancer or other conditions. It helps relieve jaundice and other symptoms.
Ureteral Stents
Ureteral stents are placed in the ureters to ensure the flow of urine from the kidneys to the bladder. They are commonly used to treat blockages caused by kidney stones or other conditions. This helps prevent kidney damage and relieve pain.
How Stents Work in the Body
Stents are vital for keeping the heart healthy by providing mechanical support and sometimes delivering medication. It’s key to understand how stents work to see their role in treating heart conditions.
Mechanical Support Mechanism
The main job of a stent is to keep the artery open, ensuring blood flows well. This is critical in cases of coronary artery disease, where plaque can narrow arteries.
- Stents expand when put in, pressing against the artery walls.
- They’re made from metal mesh or other materials to handle artery pressures.
- The stent’s design keeps the artery open, lowering the chance of it narrowing again.
Drug Delivery Systems
Some stents have drug delivery systems to prevent complications like in-stent restenosis. These drug-eluting stents (DES) cut down the risk of re-narrowing more than bare-metal stents.
- Drug-eluting stents have a polymer coating that releases medication slowly.
- The drugs, like antiproliferative agents, stop cell growth that could cause re-narrowing.
- The controlled drug release keeps the artery open, boosting patient outcomes over time.
Modern stents combine mechanical support with drug delivery. This approach offers a complete solution for heart disease, improving patients’ lives significantly.
The Complete Stent Procedure Process
The stent procedure involves several key steps, from initial evaluation to post-procedure care. It’s vital for patients to understand each stage. This knowledge helps them feel more informed and prepared.
Pre-Procedure Evaluation and Testing
Patients undergo a detailed evaluation before the procedure. This includes blood tests, electrocardiograms, and imaging studies like angiograms. These tests help doctors decide the best stent placement approach.
Angioplasty and Stent Placement Technique
Angioplasty is performed first to widen the narrowed artery. A catheter with a balloon is inserted, and the balloon is inflated to compress the plaque. Next, a stent is placed to keep the artery open. The stent is carefully positioned and expanded for optimal blood flow.
Immediate Post-Procedure Monitoring
After stent placement, patients are monitored in a recovery area for hours. Medical staff check for complications and ensure the stent is working right. Patients might feel soreness or bruising at the catheter site, but this usually goes away quickly.
Hospital Discharge Protocol
When patients are stable, they are discharged with care instructions. They receive details on medication, activity levels, and follow-up appointments. Following these instructions is critical for a smooth recovery and effective stent function.
Benefits of Stent Placement
Stent placement has transformed the treatment of cardiovascular diseases, bringing numerous advantages to patients globally. It has become a key method for managing vascular conditions, providing a safe and effective solution. This procedure has significantly impacted the lives of many, making it a cornerstone in modern medicine.
Improved Blood Flow and Circulation
Stent placement’s primary advantage is restoring normal blood flow. By maintaining the artery’s openness, stents ensure oxygen-rich blood reaches the heart or vital organs. This is vital for those with coronary or peripheral artery disease, improving circulation and overall health.
Symptom Relief and Quality of Life
Stent placement often brings significant symptom relief, boosting patients’ quality of life. For example, those with coronary artery disease may see a decrease in angina symptoms. Patients with peripheral artery disease may notice better walking distances and less pain.
Minimally Invasive Alternative to Open Surgery
Another key benefit is its minimally invasive nature. Unlike open-heart surgery, stent placement requires smaller incisions and less tissue damage. This results in shorter recovery times, appealing to those at high risk for complications from more invasive surgeries.
In summary, stent placement offers substantial benefits for treating cardiovascular diseases. It enhances health outcomes and improves the quality of life for patients, making it a valuable treatment option.
Potential Risks and Complications of Stents
Stent placement is a highly effective procedure, but it comes with risks and complications. These can vary based on the patient’s health and the condition being treated. Understanding these risks is essential.
Procedure-Related Complications
Complications can happen during or right after stent placement. These may include:
- Bleeding at the access site
- Blood vessel damage
- Allergic reactions to the contrast dye used during the procedure
While rare, it’s vital to monitor patients closely during and after the procedure.
Short-Term Risks
Short-term risks include:
- Blood clots forming on the stent
- Infection at the access site
These are usually managed with medication and close monitoring.
Long-Term Concerns
Long-term concerns include:
- The development of in-stent restenosis
- Stent fracture or migration
Regular follow-ups with a healthcare provider are key to monitoring these issues.
In-Stent Restenosis: Causes and Prevention
In-stent restenosis is a significant concern. It’s caused by:
- Neointimal hyperplasia (growth of new tissue)
- Stent underexpansion
Prevention involves using drug-eluting stents and following antiplatelet therapy.
Recovery After Stent Placement
Understanding the recovery process after stent placement is key to improving the patient’s quality of life and the procedure’s success. The recovery period includes several important aspects. Patients need to be aware of these to ensure a smooth and effective healing process.
First Week After Procedure
The first week after stent placement is critical. Patients are monitored for a few hours post-procedure and may spend the night in the hospital for observation. During this time, soreness or bruising at the catheter insertion site is common.
Activity Restrictions and Gradual Return
Patients are advised to avoid heavy lifting, bending, or strenuous activities for a few days to a week. A gradual return to normal activities is recommended, with most patients resuming their routines within a week. It’s essential to follow the specific instructions from the healthcare provider.
Follow-Up Care Schedule and Importance
Follow-up care is vital after stent placement. Patients typically have a follow-up appointment with their doctor within a few weeks. This appointment is to check on healing progress and discuss any concerns or symptoms. Adhering to the follow-up care schedule is critical for ensuring the stent is functioning correctly and addressing any issues early.
Essential Medications After Stent Placement
After stent placement, patients are given a set of essential medications. These ensure the stent works right and prevent complications. They are key to recovery and the success of the procedure.
Dual Antiplatelet Therapy (DAPT)
Dual Antiplatelet Therapy (DAPT) is vital for patients with drug-eluting stents. It uses two antiplatelet drugs to stop platelets from clumping. This prevents blood clots that could block the stent.
Aspirin Regimen
Aspirin is a key part of DAPT. It stops platelets from sticking together by blocking thromboxane A2 production. Patients usually take 81 mg of aspirin daily, but dosage can vary.
P2Y12 Inhibitors
The other part of DAPT is a P2Y12 inhibitor, like clopidogrel or ticagrelor. These drugs block the P2Y12 receptor on platelets. The choice and duration of these drugs depend on the stent type and patient risk.
Statins and Cholesterol Management
Statins are also important after stent placement. They lower cholesterol and reduce cardiovascular risk. By managing cholesterol, statins help ensure the stent’s long-term success.
- Atorvastatin
- Rosuvastatin
- Simvastatin
These statins are commonly used, each with its own strength and side effects. The right statin and dosage are chosen for each patient.
Medication Compliance and Possible Interactions
Following the medication plan is critical for stent success. Not taking medications as directed can lead to serious issues. Patients should tell their doctors about all medications and supplements they use.
Understanding these medications and talking openly with healthcare teams is essential. This helps patients recover well and achieve long-term success after stent placement.
Lifestyle Changes with a Stent
Receiving a stent marks a critical juncture for cardiovascular health. It necessitates a shift towards a healthier lifestyle. This entails making significant adjustments to daily habits and routines.
Heart-Healthy Diet Recommendations
Post-stent placement, a heart-healthy diet becomes indispensable. Focus on consuming fruits, vegetables, whole grains, and lean proteins. It’s equally important to restrict saturated fats, trans fats, and cholesterol.
Opt for healthy fats in avocados and nuts. Reduce sodium intake and drink plenty of water to stay hydrated.
Safe Exercise Guidelines and Cardiac Rehabilitation
Regular physical activity is essential for heart health post-stent. It’s vital to adhere to safe exercise guidelines. Begin with low-intensity activities and gradually increase intensity and duration.
Cardiac rehabilitation programs are highly recommended. They offer a structured exercise plan and support from healthcare professionals. These programs aid in regaining strength, improving cardiovascular health, and reducing future heart risks.
Smoking Cessation and Stress Management
Quitting smoking is a critical lifestyle change post-stent. Smoking cessation programs and resources are invaluable in this journey.
Stress management is equally vital for heart health. Techniques like meditation, deep breathing, and yoga can help. Identifying and addressing daily stressors is also beneficial.
Stent Technology Advancements and Innovations
Stent technology has seen major leaps forward, thanks to breakthroughs in materials science and bioengineering. These advancements are making stents safer, more effective, and better at treating cardiovascular diseases.
Evolution of Stent Materials and Design
New stent materials and designs have been a key focus. Alloys like cobalt-chromium and platinum-chromium are stronger and more visible, allowing for thinner struts and easier delivery. Also, designs like helical stents and those with variable strut thickness aim to improve flexibility and fit against the vessel wall.

Smart Stents with Monitoring Capabilities
Smart stents with sensors for real-time monitoring mark a major leap. They can track pressure, temperature, or biochemical changes, spotting issues like restenosis or thrombosis early. This could change how we manage stents post-procedure and boost patient results.
Biodegradable and Bioabsorbable Technologies
Biodegradable and bioabsorbable stents offer a new approach. They act as temporary supports and then dissolve, aiming to cut down on long-term issues with permanent stents. Materials like poly-L-lactic acid (PLLA) are being tested, showing early promise in trials.
The ongoing evolution in stent technology is a beacon of hope for better cardiovascular disease treatment. It promises safer, more tailored, and effective care for patients.
Cost and Insurance Considerations for Stent Procedures
Stent procedures are lifesaving but come with a significant cost. This cost varies based on several factors, including location, stent type, and medical facility charges. It’s vital for patients to understand these costs and how insurance covers them.
Average Procedure Costs in the United States
In the United States, the average cost for a stent procedure can range from $20,000 to $50,000 or more. This figure includes the stent, procedure, hospital stay, and follow-up care. The actual cost can vary based on the procedure’s complexity and the hospital’s billing practices.
Medicare and Private Insurance Coverage
Most health insurance plans, including Medicare, cover stent procedures when deemed medically necessary. Medicare Part A covers the hospital stay, while Part B covers the doctor’s services and outpatient care. Private insurance plans differ in their coverage, making it critical for patients to review their policies.
- Medicare coverage includes:
- Hospital stay under Part A
- Doctor’s services and outpatient care under Part B
- Some Medicare Advantage plans may offer additional benefits
Financial Assistance Programs and Resources
For those facing financial challenges, numerous assistance programs are available. These include hospital financial aid programs, non-profit organizations providing grants, and government assistance for eligible individuals.
- Hospital financial aid programs
- Non-profit organizations
- Government assistance programs
When to Contact Your Doctor After Stent Placement
After a stent is placed, it’s vital to keep a close eye on your health. Knowing when to seek medical help is key. Your doctor will give you specific instructions. Being aware of possible issues can help you react quickly.
Emergency Warning Signs
Certain symptoms need immediate attention. If you notice any of these, call emergency services or head to the nearest emergency room:
- Chest pain or discomfort that doesn’t go away
- Shortness of breath
- Severe headache or confusion
- Weakness or numbness in your face, arm, or leg
- Bleeding that doesn’t stop
Non-Emergency Concerns and Questions
For non-emergency issues, like medication side effects or swelling at the stent site, contact your doctor’s office. They can offer advice or set up an appointment if needed.
Being proactive in your post-stent care can greatly influence your recovery. Don’t hesitate to contact your healthcare provider if you have any doubts or concerns.
Living with a Stent: Real Patient Experiences
The journey of a patient with a stent is filled with challenges and triumphs that shape their daily life. Living with a stent requires adjustments, but many patients report a significant improvement in their overall health and well-being.
Quality of Life Improvements
Patients who have undergone stent placement often experience improved blood flow and reduced symptoms associated with cardiovascular disease. This improvement can lead to a more active lifestyle, allowing individuals to engage in activities they previously had to avoid due to health concerns.
For instance, a patient might find it easier to walk or exercise without experiencing chest pain or shortness of breath, significantly improving their quality of life.
Adjusting to Long-Term Management
Long-term management after stent placement involves medication adherence, lifestyle changes, and regular follow-ups with healthcare providers. Patients must adjust to a new routine that includes dual antiplatelet therapy and possibly other medications to prevent complications.
Understanding the importance of these adjustments is critical for minimizing risks and maximizing the benefits of stent placement.
Personal Stories and Perspectives
Real patient experiences vary widely, with some individuals adapting quickly to life with a stent, while others may face challenges. Hearing personal stories and perspectives can provide valuable insights and support for those navigating similar journeys.
These stories highlight the resilience and adaptability of patients and offer practical advice on managing life after stent placement.
Advancing Cardiovascular Care: The Future of Stent Technology
The future of stent technology is set to transform cardiovascular care, bringing new treatment options for those with coronary artery disease and other vascular issues. Medical research is pushing forward, leading to the development of advanced stent designs and materials. These innovations aim to enhance patient outcomes significantly.
Bioresorbable stents are a promising area of research, designed to dissolve over time after their function is fulfilled. This could lower the risk of long-term complications. Also, drug-eluting stents are being improved to better prevent in-stent restenosis, a common issue.
Smart stents with monitoring capabilities are on the horizon. These stents could offer real-time data on blood flow and pressure. This would enable more accurate monitoring and management of cardiovascular health.
The ongoing evolution of stent technology relies heavily on collaboration between cardiologists, researchers, and medical device manufacturers. Through these efforts, we can significantly improve patient lives globally. The goal is to advance cardiovascular care with cutting-edge stent solutions.
FAQ
Q: What is a stent and how does it work?
A: A stent is a small, mesh-like device inserted into a narrowed or blocked artery. It improves blood flow by providing mechanical support. In some cases, it also delivers medication to prevent complications.
Q: What are the different types of stents available?
A: There are various stents, including bare metal, drug-eluting, and bioresorbable vascular scaffolds. Each type has unique characteristics and benefits, tailored for specific applications.
Q: What medical conditions require stent placement?
A: Stents are often used for coronary artery disease, peripheral artery disease, and carotid artery stenosis. They are also used in non-vascular applications, such as biliary and ureteral stents.
Q: What is the stent procedure process like?
A: The stent procedure starts with evaluation and testing. It then involves angioplasty and stent placement. Post-procedure monitoring and hospital discharge protocols follow.
Q: What are the benefits of stent placement?
A: Stent placement improves blood flow and relieves symptoms. It enhances quality of life and is a minimally invasive alternative to open surgery.
Q: What are the risks and complications of stents?
A: Risks include procedure-related complications and long-term concerns like in-stent restenosis. Understanding these risks is essential for patient care.
Q: How long does it take to recover after stent placement?
A: Recovery typically takes a few days to a week. It involves rest, activity restrictions, and gradual return to normal activities. Follow-up care is also important.
Q: What medications are required after stent placement?
A: Medications include dual antiplatelet therapy, statins, and cholesterol management drugs. Adherence to these medications is critical to prevent complications.
Q: What lifestyle changes are necessary after stent placement?
A: Adopting a heart-healthy diet and following safe exercise guidelines are essential. Quitting smoking and managing stress also promote cardiovascular health.
Q: How do I know when to contact my doctor after stent placement?
A: Contact your doctor for emergency warning signs or non-emergency concerns and questions. Knowing when to seek medical attention is vital.